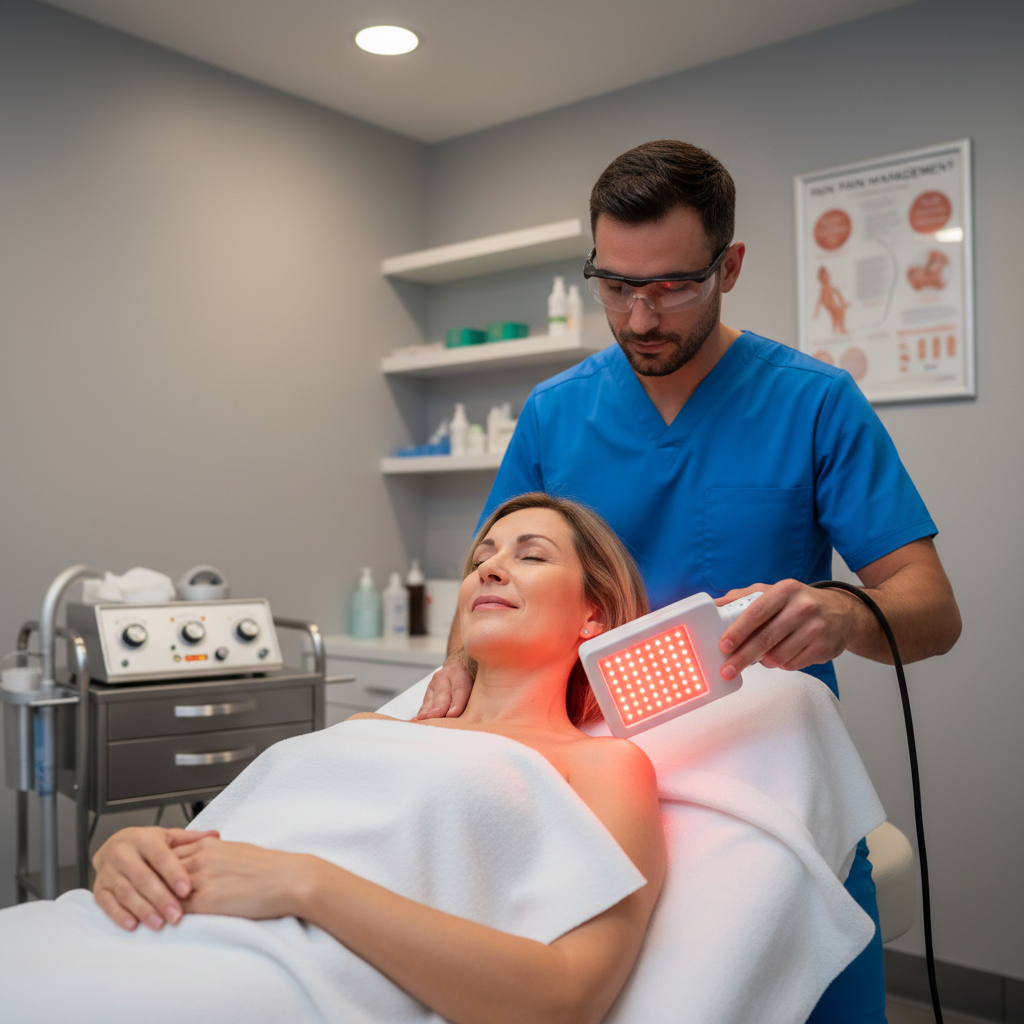
The Master Guide to Red Light Therapy for Chronic Pain
Medical Disclaimer: This content is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of a physician or other qualified health provider with any questions regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read here. If you are pregnant, have active malignancies, or use photosensitizing medications, consult a specialist before beginning photobiomodulation (PBM) therapy.
Summary
Red light therapy, or photobiomodulation (PBM), utilizes specific wavelengths of light to support cellular repair and modulate inflammatory pathways. It is increasingly recognized as a non-invasive, drug-free modality for managing chronic pain conditions such as fibromyalgia, osteoarthritis, and neuropathy. By targeting mitochondrial function and supporting ATP production, this therapy aims to address underlying biological drivers of discomfort.

Key Takeaways
- Cellular Support: PBM interacts with cytochrome c oxidase in the mitochondria, which may increase cellular energy (ATP) to support tissue repair processes.
- Inflammation Modulation: Research suggests regular application may help lower pro-inflammatory cytokines, potentially benefiting systemic conditions like rheumatoid arthritis.
- Wavelength Specificity: Efficacy is highly dependent on using appropriate wavelengths—typically 660nm for superficial tissue and 850nm for deeper joint or nerve penetration.
- The Dosing "Sweet Spot": Following the Arndt-Schulz Law is critical; both under-dosing and excessive over-dosing can lead to diminished therapeutic returns.
- Multimodal Approach: Red light therapy is most effective when integrated into a broader care plan including physical therapy and anti-inflammatory lifestyle choices.
Understanding Photobiomodulation for Chronic Pain
Chronic pain often involves a complex interplay of persistent inflammation, nerve sensitization, and reduced localized circulation. While traditional management often relies on pharmacological interventions, the clinical landscape in 2026 has shifted toward photobiomodulation (PBM) as a significant adjunctive tool. PBM delivers photons to light-sensitive molecules within cells, initiating biochemical cascades that support recovery.
Unlike surgical lasers, red and near-infrared (NIR) devices are non-thermal. They trigger biological responses rather than cutting or heating tissue. To ensure safety and efficacy, users should adhere to established safety standards and technical specifications for photobiomodulation, which define the necessary power density (irradiance) and spectral accuracy required to reach target tissues.
Biological Mechanisms: The Science of Light Interaction
The primary mechanism behind PBM is the stimulation of mitochondria. When red (660nm) or near-infrared (850nm) light is absorbed by the enzyme cytochrome c oxidase, it is believed to displace nitric oxide—a molecule that can inhibit cellular respiration during stress. This displacement allows oxygen to bind more effectively, potentially boosting Adenosine Triphosphate (ATP) production.
Increased ATP provides the energy necessary for cells to perform repair functions and maintain homeostasis. Furthermore, PBM is thought to modulate reactive oxygen species (ROS) signaling, which activates genes involved in cellular protection. For those with chronic pain, this may result in a reduction of the "inflammatory soup" that irritates nerve endings.

Evidence-Based Applications for Specific Conditions
The application of PBM varies based on the depth and nature of the pain.
Osteoarthritis and Joint Pain
Systematic reviews and clinical guidelines (such as those from WALT) suggest that NIR light (850nm) can penetrate to the synovial fluid and cartilage in joints. By potentially reducing matrix metalloproteinases (enzymes that degrade cartilage) and supporting localized blood flow, PBM may help manage the stiffness associated with osteoarthritis.
Neuropathy and Nerve Pain
Nerve pain management is a developing field for PBM. Studies indicate that light therapy may promote the expression of nerve growth factors and improve microcirculation. This is particularly relevant for diabetic neuropathy, where improved oxygenation may lead to a reduction in symptoms like tingling or numbness.
Fibromyalgia and Systemic Pain
For widespread conditions like fibromyalgia, full-body panels are often utilized. These devices aim to provide a systemic effect, potentially helping to regulate the central nervous system's pain response and improving sleep quality—a vital component of chronic pain recovery.
Expert Note: The effectiveness of PBM assumes the use of a high-quality device capable of delivering consistent irradiance. Results are individual and depend on tissue depth and baseline metabolic health.
2026 Standards for Therapeutic Dosing
Achieving results requires precision. We follow the Arndt-Schulz Law, which posits a biphasic dose-response: too little light has no effect, while too much can inhibit healing.
| Parameter | Recommended Range | Primary Purpose |
|---|---|---|
| Wavelength (Red) | 630nm - 670nm | Superficial tissue, skin health, and wound support. |
| Wavelength (NIR) | 810nm - 850nm | Deep tissue, joints, tendons, and nerves. |
| Irradiance | 50 - 100 mW/cm² | Power density required to reach target depth. |
| Fluence (Dose) | 10 - 60 Joules/cm² | Total energy delivered per treatment area. |
| Frequency | 3 - 5 times per week | Allows for cellular recovery and cumulative benefit. |
How to Calculate Your Dose at Home
To ensure you are within the therapeutic window, use this standard calculation: Dose (J/cm²) = [Irradiance (mW/cm²) × Time (seconds)] / 1000
Example: If your device delivers 50 mW/cm² at a 6-inch distance, and you treat the area for 10 minutes (600 seconds): (50 × 600) / 1000 = 30 J/cm². This falls directly within the recommended 10–60 J/cm² range for deep-tissue pain.
For technical validation, refer to the Photobiomodulation Standards: Irradiance, EMF, and Safety (Manufacturer Whitepaper), which aligns with IEC 60601-2-57:2026 safety standards.
Integrating PBM with Conventional Care
Red light therapy is most effective as a powerful adjunct to traditional medicine.
- Physical Therapy: Using PBM immediately before a session may "prime" tissues, potentially reducing movement-related pain.
- Nutrition: A diet rich in omega-3 fatty acids and antioxidants supports the repair processes triggered by light.
- Medication Management: Some patients find that consistent PBM allows for a supervised reduction in NSAID use. Never alter your medication regimen without consulting your doctor.
Long-Term Management and Safety
While the body does not develop a pharmacological "tolerance," improvements may plateau once cellular deficits are corrected. A "maintenance phase" (2-3 times per week) is often recommended after an initial 8-12 week intensive period.
When to Stop or Adjust: If you experience temporary fatigue, increased sensitivity, or "diminishing returns," you may be over-stimulating the tissue. Reduce session time or frequency.
How to Verify Device Efficacy
To avoid "irradiance inflation," use this checklist:
- Independent Lab Reports: Request third-party data for spectral output and irradiance.
- Flicker & EMF Safety: Ensure compliance with IEEE 1789-2015 to prevent eye strain or neurological stress.
- Measurement Tools: For high-precision verification, consumers can use handheld spectroradiometers (e.g., Hopoocolor series) to measure actual mW/cm² at specific distances.
- Warranty: Look for a minimum 2-year warranty, indicating build quality and manufacturer confidence.
FAQ
How long does it take to see results? While some experience temporary relief within days due to improved blood flow, biological tissue remodeling typically requires 4 to 8 weeks of consistent use.
Can I use red light therapy every day? Daily use is generally considered safe during the initial phase. However, exceeding 20 minutes per area may trigger the biphasic response, where benefits are neutralized by over-stimulation.
Is it safe for use with metal implants? PBM is non-ionizing and does not heat metal like microwave or ultrasound therapies. It is generally considered safe for those with spinal hardware or joint replacements, though consulting your surgeon is recommended.
Are there contraindications? Avoid use over active malignancies, the abdomen during pregnancy, or if you have light-sensitive epilepsy. Always check if your medications are photosensitizing.
References
Government & Regulatory Standards
- IEC 60601-2-57:2026: Safety requirements for non-laser light source equipment for therapeutic use.
- FDA (2025 Update): Product Classification for Light-Based Pain Management Devices.
Professional Associations
- World Association for Laser Therapy (WALT): Dosage Guidelines for Photobiomodulation (2024 Revision).
- ASLMS: Position Statement on the Efficacy of Home-Use PBM Devices.
Academic Research & Technical Papers
- Hamblin, M. R. (2025): "Mechanisms of Photobiomodulation: Mitochondrial Signaling." Journal of Photochemistry and Photobiology.
- Manufacturer Data: Youlumi Whitepaper: Photobiomodulation Standards: Irradiance, EMF, and Safety. (Technical specifications provided by the manufacturer).
Community Resources
- Reddit r/Photobiomodulation: User-led discussions on device setups (Informational only).
- Biohacker Forum: Independent testing of consumer-grade light meters (Informational only).