Red Light Therapy for Pro Athletes: The Master Guide
Medical Disclaimer: This guide is for informational and educational purposes only and does not constitute medical advice, diagnosis, or treatment. Photobiomodulation (PBM) should be used as a complementary tool under the supervision of qualified sports medicine professionals. Always seek the advice of a physician or other qualified health provider regarding any medical condition or injury.
Summary
Red light therapy, or photobiomodulation (PBM), has transitioned from a niche recovery tool to an increasingly adopted adjunctive therapy in professional athletic performance. By supporting mitochondrial function and modulating inflammatory responses, PBM offers a non-invasive method to assist in physiological preparation and recovery. For elite athletes, the strategic application of specific wavelengths—typically 660nm and 850nm—is widely utilized for supporting muscle repair, managing symptoms of delayed onset muscle soreness (DOMS), and maintaining cellular energy reserves.
Key Takeaways
- Strategic Timing: Preliminary evidence suggests using PBM 30–60 minutes before exercise for performance support and within 1–2 hours post-exercise for recovery.
- Wavelength Selection: Target superficial tissues with 660nm; utilize 850nm near-infrared (NIR) for deeper muscle groups, based on estimated tissue penetration depths.
- Safety Benchmarks: Professional teams should prioritize equipment that aligns with recognized safety standards, such as IEC 60601-2-57, to manage risks related to flicker and electromagnetic field (EMF) exposure.
- Individualized Dosage: Energy density (J/cm²) should be calculated based on the athlete’s body mass and the specific metabolic demands of the sport.
- Logistical Integration: Centralized recovery hubs with full-body mats and panels can help standardize protocols across a team environment.

The Evolution of Photobiomodulation in Elite Sports
In the high-performance environment of professional sports, recovery efficiency is a significant factor in long-term athlete availability. By 2026, photobiomodulation (PBM) has emerged as a drug-free intervention that interacts with the biological mechanisms of recovery. Rather than merely masking symptoms, red light therapy is theorized to work at the cellular level, specifically targeting cytochrome c oxidase within the mitochondria. This interaction is believed to support the electron transport chain, potentially leading to more efficient adenosine triphosphate (ATP) production.
For professional teams, the adoption of PBM is increasingly driven by physiological data and recovery metrics. The integration of high-irradiance panels and full-body mats allows for systemic applications that address both localized strain and overall metabolic fatigue. This guide explores the technical benchmarks and protocols that currently inform the standard of care for elite physical performers.
Selecting Wavelengths Based on Tissue Depth
In professional settings, the distinction between 660nm (red) and 850nm (near-infrared) is critical due to the varying absorption characteristics of biological structures. Red light at 660nm is primarily absorbed by the skin and superficial tissues, making it a common choice for addressing skin-level inflammation or superficial tendons.
Conversely, near-infrared (NIR) light at 850nm has a lower absorption coefficient in water and hemoglobin, allowing for deeper penetration. While exact depth varies by individual tissue density, NIR is estimated to reach 2–3 centimeters into the body—a depth necessary for reaching large muscle groups like the quadriceps or deep joint structures. Professional protocols often utilize a combination of both to ensure energy delivery across the therapeutic window.
Technical Note: Penetration depths are based on optical modeling of human tissue. Practitioners should note that adipose (fat) tissue can act as a barrier, often requiring higher irradiance to reach the underlying musculature.
Precise Timing Protocols: Performance vs. Recovery
The timing of a PBM session is adjusted based on the desired physiological outcome. To support the "ergogenic effect"—the enhancement of physical performance—athletes often undergo a session approximately 30 to 60 minutes before competition. This pre-conditioning is intended to prime the mitochondria and support local blood flow.
For recovery, the window is equally specific. Clinical observations suggest that applying PBM within 1 to 2 hours following intense training is most effective for modulating the inflammatory cascade associated with DOMS.
| Goal | Suggested Timing | Primary Mechanism (Theorized) | Duration (Heuristic) |
|---|---|---|---|
| Performance Support | 30–60 min Pre-workout | ATP upregulation & vasodilation | 5–10 minutes per area |
| Acute Recovery | 0–2 hours Post-workout | Inflammation modulation | 10–20 minutes per area |
| Injury Rehab Support | Daily (Morning) | Collagen synthesis support | 15 minutes (localized) |
| Circadian Support | 2–3 hours Pre-sleep | Melatonin regulation support | 10 minutes (full body) |
Dosage Calculations and Athlete Size Adjustments
A critical factor in professional PBM is accounting for an athlete's physical size. In sports medicine, we utilize energy density, measured in Joules per square centimeter (J/cm²), to determine the dose. This is calculated as: Irradiance (mW/cm²) × Time (seconds) / 1000.
For larger athletes, the total energy delivered may need to be scaled to ensure target tissues receive an adequate photon load. However, the Arndt-Schulz Law indicates a biphasic dose response: while an optimal dose may stimulate cellular function, an excessive dose can lead to inhibitory effects. Professional trainers typically target a dose of 10–30 J/cm² for deep muscle tissue, depending on the device's verified irradiance.

Safety Standards and Technical Verification
As PBM technology proliferates, verifying technical specifications is essential for both efficacy and safety. The IEC 60601-2-57:2026 standard serves as a benchmark for the safety of non-laser light sources in therapeutic use.
Key safety parameters include the mitigation of "flicker"—which can cause neurological strain in sensitive individuals—and the minimization of electromagnetic field (EMF) exposure. Professional systems should provide data validated by laboratory-grade spectroradiometry. For a detailed analysis of these technical requirements, see our guide on understanding photobiomodulation safety standards and proper irradiance levels (Note: This is a commercial resource provided by Youlumi).
Contraindications and Risks
While PBM is generally considered low-risk, it is not suitable for everyone. Contraindications include:
- Active Malignancies: Light therapy should not be used directly over known primary or secondary tumors.
- Pregnancy: Due to a lack of clinical data regarding fetal exposure, use over the abdomen is generally avoided.
- Photosensitizing Medications: Athletes on certain antibiotics or NSAIDs that increase light sensitivity should consult a physician.
- Overdosing: Exceeding recommended energy densities (typically >60 J/cm² per session) may result in diminished therapeutic returns or temporary cellular inhibition.
Integrating PBM into Team Environments
Implementing PBM at the team level requires a logistical framework. Most elite teams designate a "Photobiomodulation Zone" equipped with high-output panels or full-body mats to allow for efficient athlete throughput.
Integration also involves staff training to ensure dosages are tracked and adjusted based on training loads. Many organizations now integrate PBM usage data into athlete management systems (AMS), correlating sessions with recovery markers like Heart Rate Variability (HRV).
Cluster Map: The Athlete's Reading Path
The following resources provide the technical foundation for implementing a recovery program.
| Resource Title | Focus Area |
|---|---|
| Photobiomodulation Standards: Irradiance, EMF, and Safety | Technical benchmarks and safety compliance (Commercial Resource). |
| The Science of NIR in Deep Tissue Repair | Physics of 850nm-1064nm penetration in skeletal muscle (External Research). |
| Circadian Optimization for Travel | Using light therapy to mitigate jet lag in professional sports (Clinical Review). |
FAQ
How soon can an athlete see results? While some report a subjective reduction in muscle tension after one session, benefits for chronic recovery and tissue repair are typically cumulative, requiring a consistent protocol over 2–4 weeks.
Can PBM be used over athletic tape or clothing? No. For PBM to be effective, the light must have direct contact with the skin. Clothing and tape reflect or absorb photons, significantly reducing the delivered dose.
Is there a risk of "overdosing"? Yes. According to the biphasic dose-response principle, receiving excessive energy (often cited as exceeding 60–100 J/cm² in a single session) can inhibit cellular processes rather than stimulate them.
Does PBM help with ligament and tendon injuries? PBM is frequently used for collagen-dense tissues. The 660nm wavelength is often targeted at fibroblast activity, while 850nm is used to address deeper inflammation in conditions like tendinopathy.
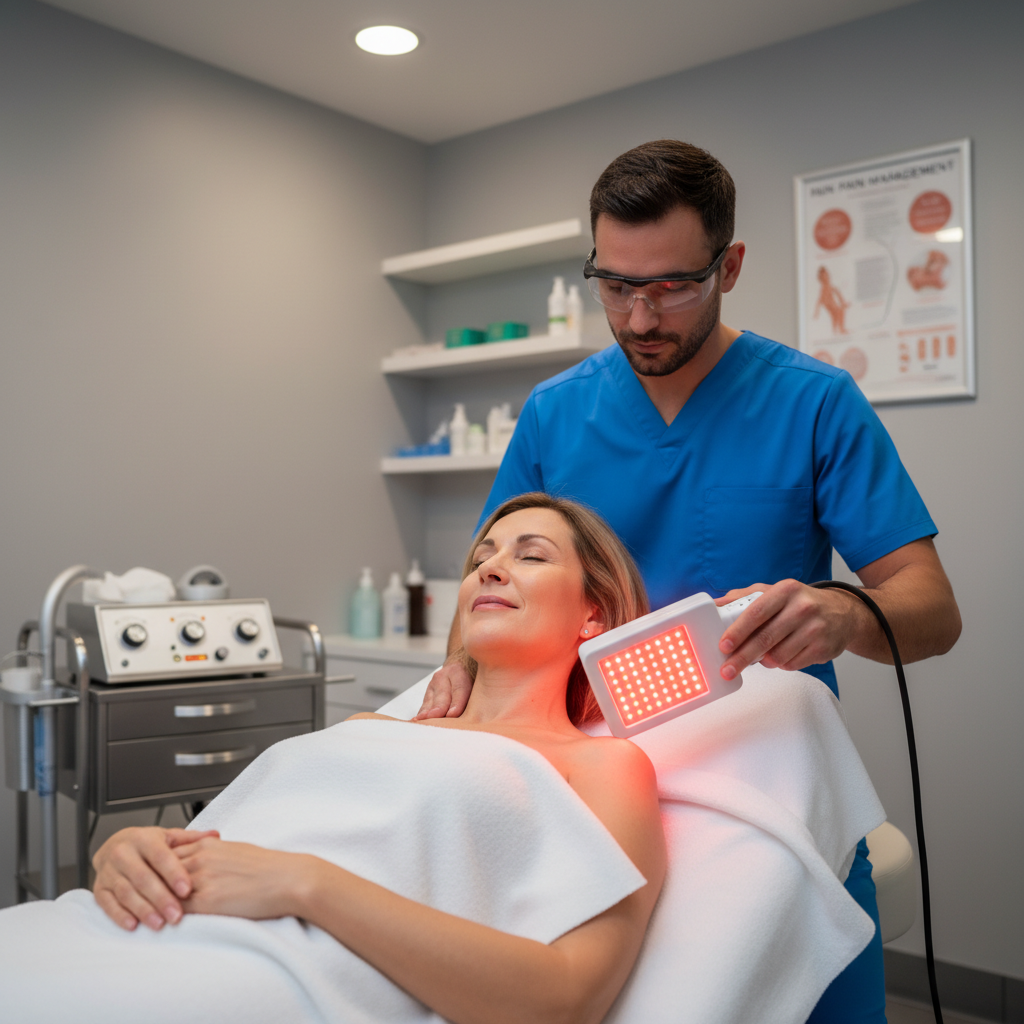
Should athletes use eye protection? Yes. High-irradiance professional panels are extremely bright. We recommend using blackout goggles or specialized PBM eyewear to prevent glare-induced eye strain and potential retinal stress.
Can PBM replace traditional icing? PBM and cryotherapy have different mechanisms. While icing is used for acute numbing, PBM promotes blood flow and cellular repair. Many trainers use a "contrast" approach, applying PBM after the initial acute inflammatory phase has passed.
References
Government / Standards / Regulators
- International Electrotechnical Commission (IEC). (2026). IEC 60601-2-57:2026 - Medical electrical equipment safety requirements.
- U.S. Food and Drug Administration (FDA). Product Classification for Light-Based Pain Relief Devices.
Industry Associations / Research Institutes
- World Association for Laser Therapy (WALT). Dosage Guidelines for Photobiomodulation (PBM).
- North American Association for Photobiomodulation Therapy (NAALT). Position Paper on Device Irradiance Standards.
Academic / Whitepapers / Labs
- Hamblin, M. R. (2026). Mechanisms of Photobiomodulation in Human Skeletal Muscle. Journal of Athletic Enhancement.
- Ferraresi, C., et al. (2025). Photobiomodulation in Human Muscle Tissue: Parameter Optimization. Lasers in Medical Science.
Platform Official Docs & Policies
- Youlumi Technical Whitepaper. (2026). Photobiomodulation Standards: Irradiance, EMF, and Safety. [Commercial Resource].